Understanding the Retina
The retina is a fundamental structure of the eye that’s responsible for visual stability. Damage to the retina can result in a series of problems. Patients with diabetes need to be extra cautious regarding retinal eye problems. Moreover, they should seek regular eye exams to monitor the impact of this disease. If you need immediate attention or would like a second opinion. The retina eye doctors at Regional Eye Associates welcome you to contact us immediately.
What is the Retina?
The retina is a significant part of the eye that helps with vision. When you see, your eyes work to convert light into signals. These are signals that the brain then interprets and turns into the images you see.
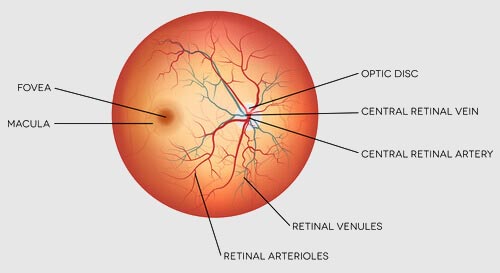
This takes place in the retina, which is located in the back of the eye. The retina is the sensory membrane that lines the inner surface of the back of the eye.
The retina has several layers and contains millions of light-sensitive cells. These cells are called rods and cones. Those rods and cones sense the image as different intensities of light and color.
When light hits the rods or cones, your body transmits signals along the brain’s nerve centers. In order to, interpret the information of the image in the retina. Then, the brain assembles those signals to allow us to see what is before us.
Other Important Definitions for Understanding the Retina
What is a Retina Specialist?
Regional Eye Associates is proud to offer a retina specialist among our staff of qualified physicians. A retina specialist is a medical doctor trained as an ophthalmologist. One who has not only received additional fellowship training in diseases. But also, in surgery of the vitreous and retina.
Retina Specialist
Gary J. Miller, MD, is the retina specialist at Regional Eye Associates. Dr. Miller joined Regional Eye Associates in 2011. He not only specializes in diabetic eye disease. But also, macular degeneration, retinal detachment, macular holes, and many other vitreoretinal diseases.
Dr. Miller has successfully treated patients with retinal disorders and diseases. He is also an expert on conditions of the retina. He develops a personalized treatment plan for each patient. While using his medical expertise combined with the latest technology available for treatment.
What are Retina Problems I Should Know About?
There is a wide variety of retina conditions, problems, and diseases. If you are concerned you may be experiencing any of these conditions or diseases. Make an appointment at Regional Eye Associates in Morgantown with one of our expert ophthalmologists.
Diabetic Retinopathy
Diabetes can cause many health problems. Including, diabetic retinopathy. There are two main stages of diabetic retinopathy.
The first is non-proliferative diabetic retinopathy (NPDR). And, the later stage is proliferative diabetic retinopathy (PDR). Diabetic retinopathy occurs when the blood vessels in the retina deteriorate due to high blood sugar levels.
When this happens, the blood vessels begin to swell and leak. Which, leads to significant vision loss if it’s left untreated. However, with early diagnosis and treatment, patients can avoid further vision loss
Macular Degeneration
The most common age-related eye disease is age-related macular degeneration (AMD). Which, affects an estimated 9 million Americans a year. This condition is the leading cause of vision loss in people who are 50 or older.
Macular degeneration is the deterioration or breakdown of the eye’s macula. Which, causes vision problems. When you have AMD, you lose your central vision. Meaning you can’t see fine details. But, you’ll still be able to use your peripheral vision without a problem.
Macular Edema
Macular edema occurs when there is fluid or swelling of the macula or central portion of the retina opposite the lens. It may also include fluid that collects underneath the macula. When this happens, it causes distortion and blurred vision. Macular edema has several causes. Including, diabetes. Which can occasionally occur after cataract surgery
Macular Hole
A macular hole can occur when there is a small break in the macula. The macula is located in the center of the eye’s light-sensitive tissue. Which is the retina. You can treat a macular hole with a vitrectomy.
Having a vitrectomy involves putting a gas bubble in the eye and removing the vitreous gel in the eye. This flattens the macular hole and keeps it in place while your eye heals.
The gas bubble will go away on its own. After a vitrectomy, you must remain facedown for a week or more. This is the only way to ensure the gas bubble remains in place while you’re healing.
Flashes & Floaters
For most people, flashes and floaters are a normal part of what they see. These are the spots or lines that seem to float in your field of vision.
If you start seeing unexpected flashes of light in your peripheral vision. This could be a sign of a problem with your retina. You may see them accompanied by floaters or floating spots. Or lines that show up in your field of vision.
Seeing unexpected flashes of light could not only signify conditions like retinal detachment. But also, macular degeneration or vitreous detachment. See an eye doctor as soon as possible to determine the cause.
Retinal Detachment
A retinal detachment is considered a medical emergency. It occurs when the retina pulls away from the back of the eye.
A surgeon must surgically reattach the retina as soon as possible if this happens. If left untreated, a retinal detachment can result in permanent vision loss.
Want more information about how to treat a retinal condition? Schedule an appointment with Regional Eye Associates today.